Chronic disease has been quietly waging war on American lives throughout the entire 21st century, quickly rising to the top of the most common causes of death in the United States. Some of the major chronic diseases, such as heart disease, chronic lung disease, and type 2 diabetes, are preventable, yet 6 out of 10 American adults still have at least one chronic disease and 4 out of 10 suffer from two or more chronic diseases. Furthermore, the prevalence of chronic diseases crushes our healthcare system with a confounding $3.8 trillion in annual healthcare costs, leading chronic disease to act as a tremendous drain on both staffing and financial resources.
Want to learn more about providing and getting paid for preventive services? Check out our detailed guide!
In response to accessibility issues and the often-unattainable cost of healthcare, President Obama and lawmakers launched an attack on chronic disease in 2010 when they enacted the Affordable Care Act (ACA). The ACA was intended to create comprehensive healthcare reform with the aim of making health insurance more affordable and available to more people than ever before. One of the key components of the ACA was the required coverage of preventive healthcare services, which aimed to help the healthcare system finally gain an upper hand on out-of-control chronic disease costs. While most payers understood the importance and cost-effectiveness of leveraging billable medical services to prevent chronic disease, some payors still restricted coverage. This resulted in patients not receiving preventive services due to the associated out-of-pocket expenses. After enactment, preventive services under the Affordable Care Act became available to millions of Americans who previously didn't have access. The resulting effect is helping American's live healthier lives through prevention and avoiding further progression of debilitating chronic diseases.
Role of the ACA in Chronic Disease Prevention and Management
Historically, payers have taken a fee-for-service approach to care. This triggered payment for practitioners after a patient was seen for a visit and a service(s) was rendered. This payment model encourages quantity over quality, creating a reactive approach to healthcare that does little to encourage the provision of preventive services. In fact, one could argue it does the opposite as unwell patients are more likely to require services.
For patients fortunate or wealthy enough to have medical insurance coverage, a visit with their primary practitioner would typically still result in some out-of-pocket cost — a figure that was sometimes significant. This would often lead patients to only seek medical care when they needed it, thus further discouraging the use of preventive services.
The enactment of and inclusion of preventive services in ACA is helping to redirect this previous trend of reactive medicine by creating a more prevention-focused approach. Such an approach, consequently, helps decrease the overall cost and increase the effectiveness of the American healthcare system. Best of all, providing preventive care access to nearly all Americans could save more than 100,000 lives annually, thus leading to better financial health for the entire country.
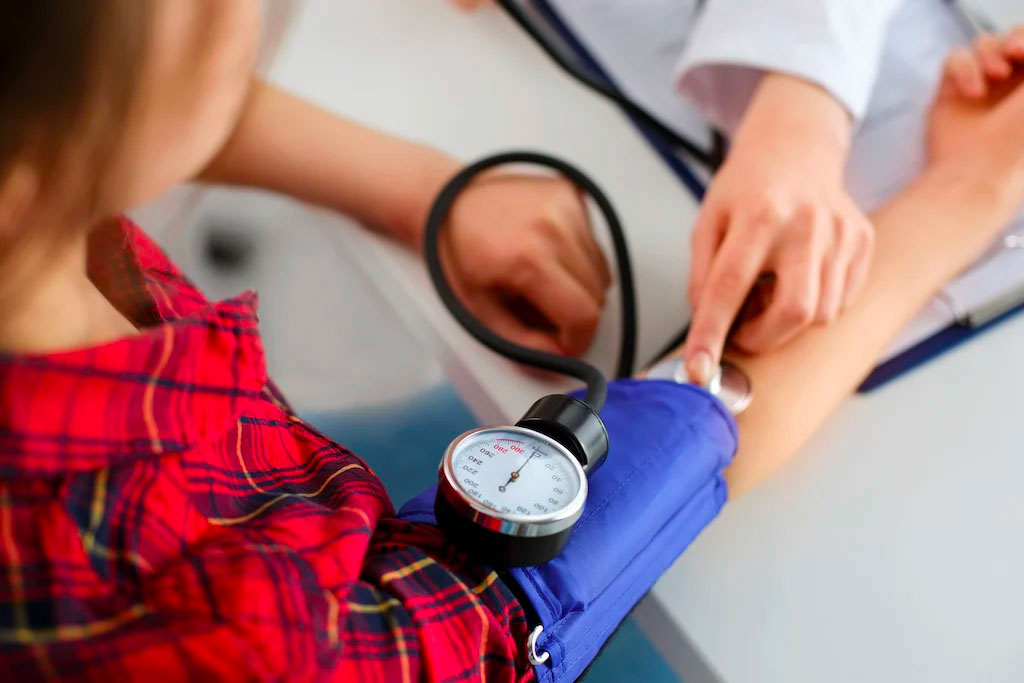
More good news: preventive services covered by the ACA are numerous and available to private payer- and public payer-covered patients typically at no out-of-pocket cost when conducted at the appropriate recommended intervals. While there are more than 20 Medicare-covered preventive services, some of the most common preventive services as outlined by the ACA include annual wellness exams, blood pressure screenings, cholesterol screenings, immunizations, diabetes screenings, depression screenings, and colorectal cancer screenings. Many of the preventive services in ACA have specific age requirements that trigger coverage eligibility, so it's important that patients and practitioners understand coverage guidelines. Above all, the aim of ACA-covered preventive services is to help prevent or mitigate the effects and further progression of chronic disease.
ACA: Impact of Technology on the Provision of Chronic Disease Preventive Services
While the Affordable Care Act mandated the provision of covered preventive services, it was largely up to payers and time-strapped practitioners and their teams to figure out how best to implement the new preventive care guidelines. Fortunately, health technology companies also recognized the increased need for creative support, and many have stepped up to the plate to deliver simple and cost-effective solutions. Practitioners who use technology to support the delivery of ACA-mandated preventive services are finding themselves and their staff with more available time in their day and are better assured that they will receive accurate reimbursements.
While many health IT companies offer broad solutions for medical recordkeeping or billing, others are offering more targeted services like those designed to specifically support the provision of preventive services under the ACA. Through these health technology companies and their software solutions, practitioners and their team can find support for the preventive care services they need to deliver and help them navigate often-confusing and ever-evolving guidelines.
For example, Prevounce is one such company offering practitioners an easy way to help ensure they meet all the mandatory guidelines of the ACA. The Prevounce platform provides support for the provision of such services as:
- Advanced care planning
- Depression screening
- Alcohol abuse screening and counseling
- Smoking cessation counseling
- Obesity counseling
- Cardiovascular risk counseling
- Opioid risk assessments
- Medication therapy management
- Cognitive impairment screening
- Chronic care management
- Behavioral health integration
For busy organizations, finding the right technological support can mean all the difference. The world of stringent healthcare rules and regulations, such those put forth by the Affordable Care Act, creates an environment that breeds stress, overworking, and practitioner and staff burnout. Technology solutions can help alleviate stress and confusion while supporting practitioners' efforts to deliver great preventive care to more patients and get paid appropriately for their services.
Above all, patients and practitioners can rest assured that preventive services are not being overlooked. Technology providers are working to help with some of the most time-consuming legwork associated with the delivery of preventive services, such as pre-visit outreach and insurance and individual requirements eligibility checks. Some solutions provide step-by-step guided templates for easy medical recordkeeping. The end results: happy and healthier patients and practitioners.
Ensuring Preventive Services Within the ACA Are a Win-Win for Everyone
As the prevalence of chronic disease rose to the forefront of concern within the American healthcare system, it quickly became apparent that doing the same old thing in the same old way was no longer keeping Americans healthy. Healthcare was becoming out of reach for many Americans as the cost of care climbed. At the same time, people were becoming sicker, suffering from the very chronic health conditions that acted as a big driver in the out-of-control costs associated with our healthcare delivery system.
While many of the changes brought about through the enactment of the Affordable Care Act were confusing and challenging in the beginning, the ACA is quickly proving itself to be beneficial and even fruitful for all vested parties.
For patients, preventive services under the Affordable Care Act mean greater and more affordable access to practitioners and provide an opportunity for patients to more actively participate in their care and support living a longer, healthier life. For payers, healthier patients equate to higher profits and lower expenditures. Lastly, the ACA has given practitioners the chance to realign the care they deliver to their patients, encouraging them to address and treat the root causes of chronic disease. Even better, the ACA offers monetary incentives to keep patients healthy through the provision of preventive care, driving down the overall cost of healthcare and keeping more money in both patient's and practitioner's pockets.